As health plans shift toward digital quality measurement, Health Risk Assessment (HRA) data has never been more important. Traditionally viewed as a compliance requirement, HRAs are now a critical source of clinical and social information that can directly influence quality outcomes. With the industry’s move to electronic clinical data systems (ECDS) and greater emphasis on whole-person care, the insights captured in HRAs — from preventive screenings to social determinants of health — provide plans with actionable intelligence that goes far beyond claims data.
We’re exploring why HRAs remain indispensable even in an AI-driven world, how self-attested data supplements automated, claims-based tools and how to maximize HRAs with the right type of survey and leveraging incentives. Together, these strategies highlight the evolving role of HRAs as market dynamics, budgets and regulations shift.
Why HRAs (still) matter
Even as tech evolves and there are new, faster, automated ways to collect and aggregate member health data, HRAs are still essential tools that help members take an active role in their health, enable timely intervention and support broader initiatives to enhance population health and overall well-being. This early data capture sets the stage for:
- Identifying care gaps
- Improving risk adjustment
- Elevating quality strategies
- Enhancing member experience
Health plans see an increase in condition identification through HRA self-reported data, offering a clearer view of population health trends. This insight supports better evaluation of wellness initiatives and enables more strategic resource planning to address identified health concerns.
But not all HRAs deliver the same value. For maximum impact, the assessment must be comprehensive, accessible and aligned with regulatory and social standards. Conducting an HRA early in the plan year or at the point of enrollment provides health plans with actionable data to drive proactive care and personalized outreach. Timing and completion are key. Health plans should prioritize educating members on the importance of the HRA and implement strategies to encourage participation. A well-timed, well-executed HRA isn’t just a form, it’s a foundation for better care and greater equity.
How HRAs supplement AI tools
Health plans can and should be evaluating artificial intelligence (AI) tools to improve efficiency and outcomes, and reduce costs. However, self-reported data remains critical even in an era of AI and advanced analytics for several key reasons:
- Captures what claims and electronic health records (EHR) can’t: Administrative data, claims and EHRs provide a clinical snapshot but often miss behavioral, functional and social determinants of health (SDOH) information. Self-reported data fills these gaps, providing insights into lifestyle, social needs, mental health and patient goals.
- Enables personalized care: AI can process large datasets and predict risks, but the predictions are only as good as the input data. Self-reported information gives context and nuance that models can’t infer from structured data alone, making interventions more precise and meaningful.
- Improves member engagement: Collecting self-reported data demonstrates that the plan values the member’s voice. This engagement fosters trust, encourages adherence to care plans, and positively impacts CAHPS and other experience measures.
- Supports regulatory and quality requirements: Many measures rely on information that can only come from members themselves, such as functional status, depression screenings and social needs.
- Enables AI to work better: AI thrives on complete, high-quality data. Self-reported information supplements claims, EHR and device data, creating richer datasets that improve predictive models and actionable insights.
In short, self-reported data provides the human context that AI alone cannot capture, making it indispensable for risk stratification, quality improvement and personalized care.
Choose the right HRA
Not all HRAs are created equal. To overcome the manual, costly processes with data entry, consolidation, analysis and intervention, payers need an HRA integrated that’s integrated with the right platform. At Healthmine, we partner with health plans to implement timely, comprehensive HRAs that not only meet compliance standards but also drive meaningful insights, targeted interventions and progress toward gap closure, preventive care and health equity.
The true value of an HRA comes from how plans act on the results. Healthmine’s NCQA-certified HRA is available in both digital and print formats to meet plan and member preferences. Responses flow automatically into Healthmine’s Quality Relationship Management™ (QRM®) dashboards, regardless of if the member completed it digitally, or via mail or phone, eliminating manual data entry and boosting response rates. This allows health plans to spend less time on administrative tasks and more time leveraging actionable insights and delivering meaningful interventions to improve care. By using members’ insights to guide screenings, plan benefit design, care management, social support, or personalized outreach, plans show they are listening and responsive.
Invest in higher completion rates
So what if the member doesn’t complete an HRA? We know that often the members who need the most support are the least responsive. Healthmine’s platform delivers incentives for completion of any health action you choose, including HRA completion.For SNP plans in particular, high HRA completion rates are especially important because they directly impact the Care Management Star measure.
The 2025 Star Ratings reflect a broad upward shift in Care Management performance across all Star levels:
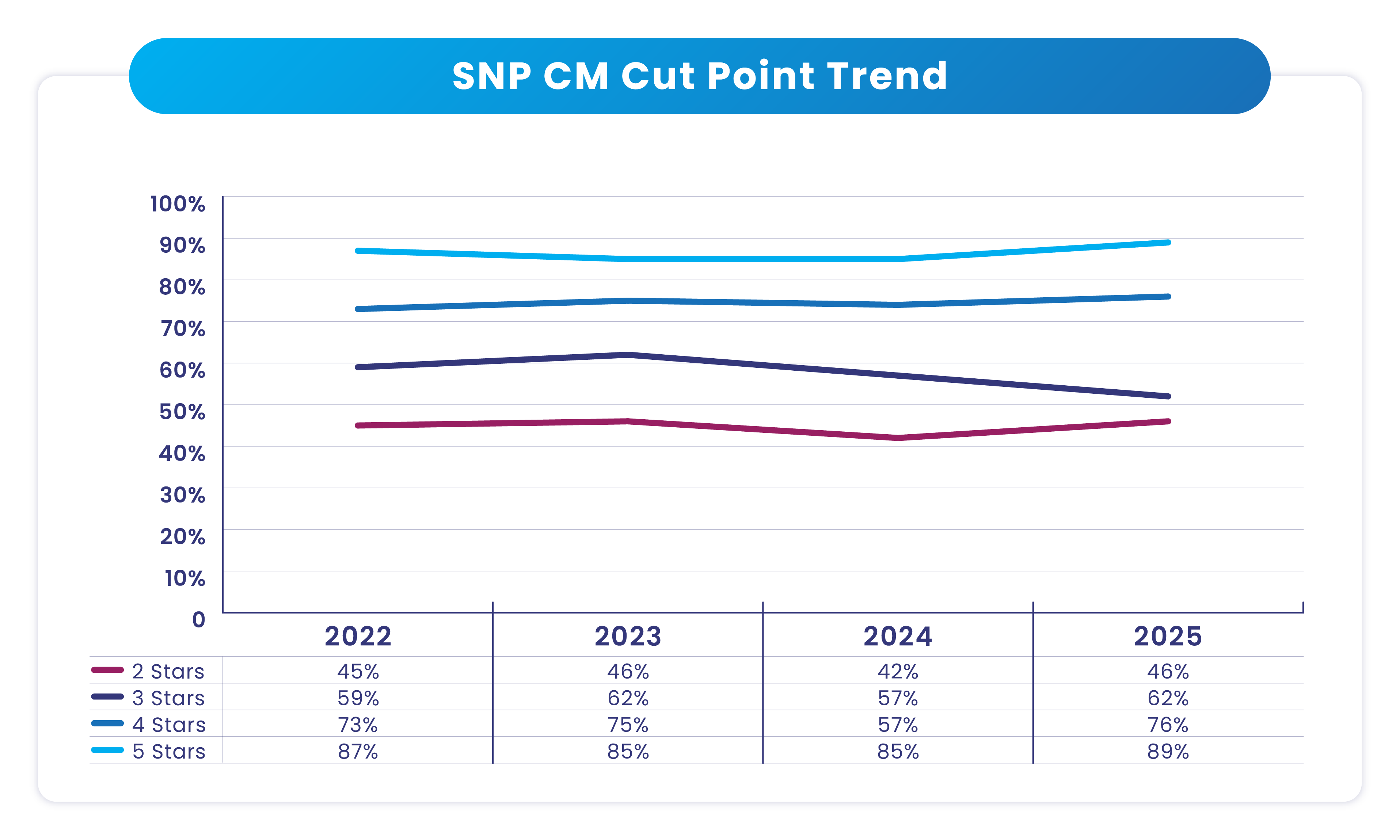
High completion rates not only ensure compliance with CMS requirements but also provide the actionable member insights needed to close gaps in care, address social determinants of health and guide individualized care planning. Since this measure influences overall Star Ratings, improving HRA participation can have a direct impact on a plan’s quality performance. Offering an incentive for completing an HRA is one of the most effective ways to boost member participation.
Incentives not only drive higher engagement by motivating members to act, but they also signal that the plan values their time and input. This simple step can be especially impactful in reaching populations that are traditionally harder to engage, ensuring more diverse and representative data. With higher completion rates, health plans gain richer insights into member risks and needs, enabling more targeted interventions and improved outcomes. In this way, incentives transform the HRA from a routine task into a meaningful touchpoint that benefits both members and plans. Incentivizing HRAs doesn’t just improve completion rates it sets the tone for stronger member relationships, which directly influences CAHPS results.

.svg)


.svg)











