One platform that actually does it all
Designed by regulatory experts to help you meaningfully connect with your members to improve outcomes.


.png)

our solution
QRM guides you through the maze of quality and risk management, data collection, and member education so you can focus on making member moments matter.
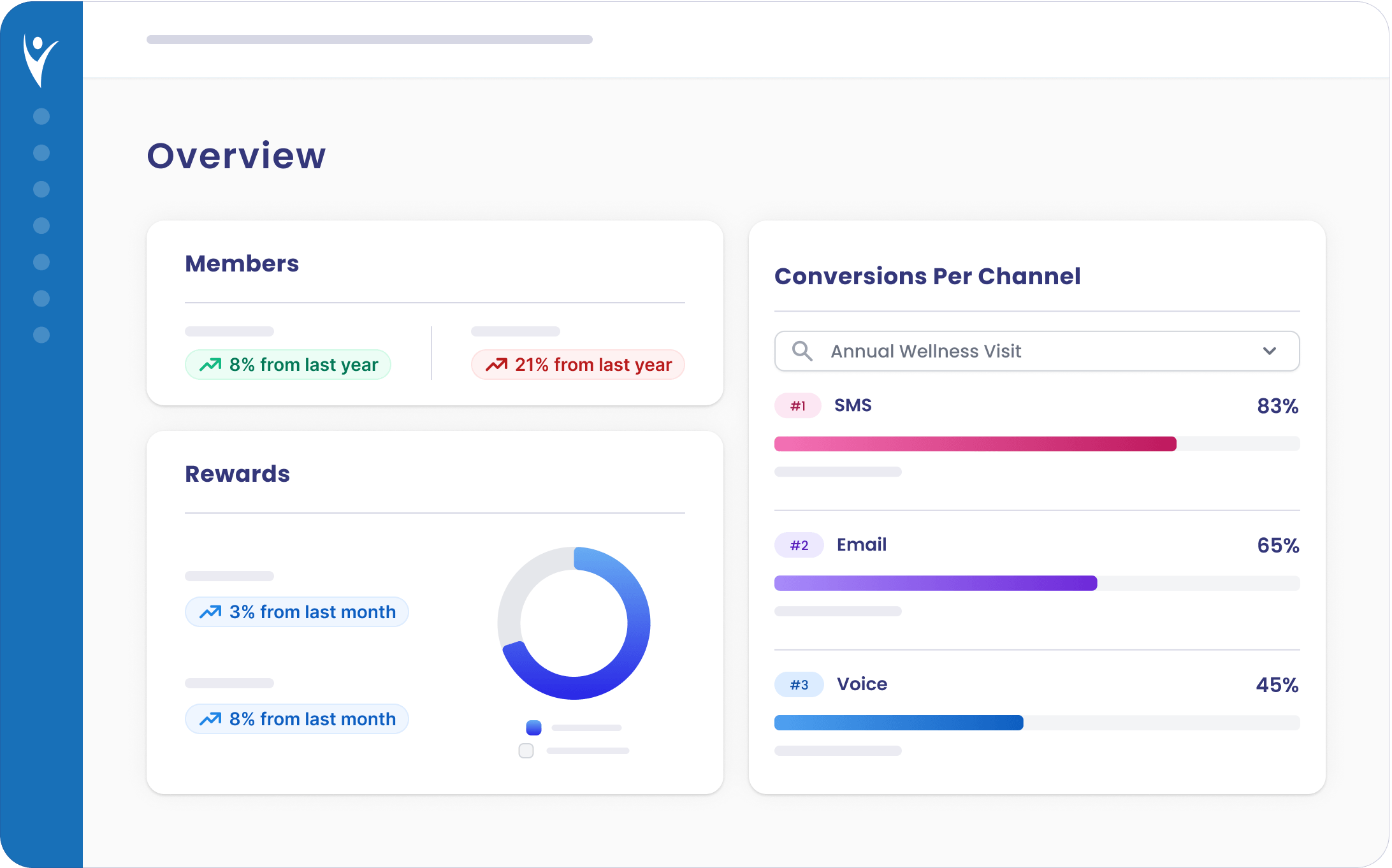
One cohesive platform
Say goodbye to multiple vendors and platforms. QRM combines omnichannel member engagement, surveying, data analysis and rewards so your team can manage every member moment in one place.
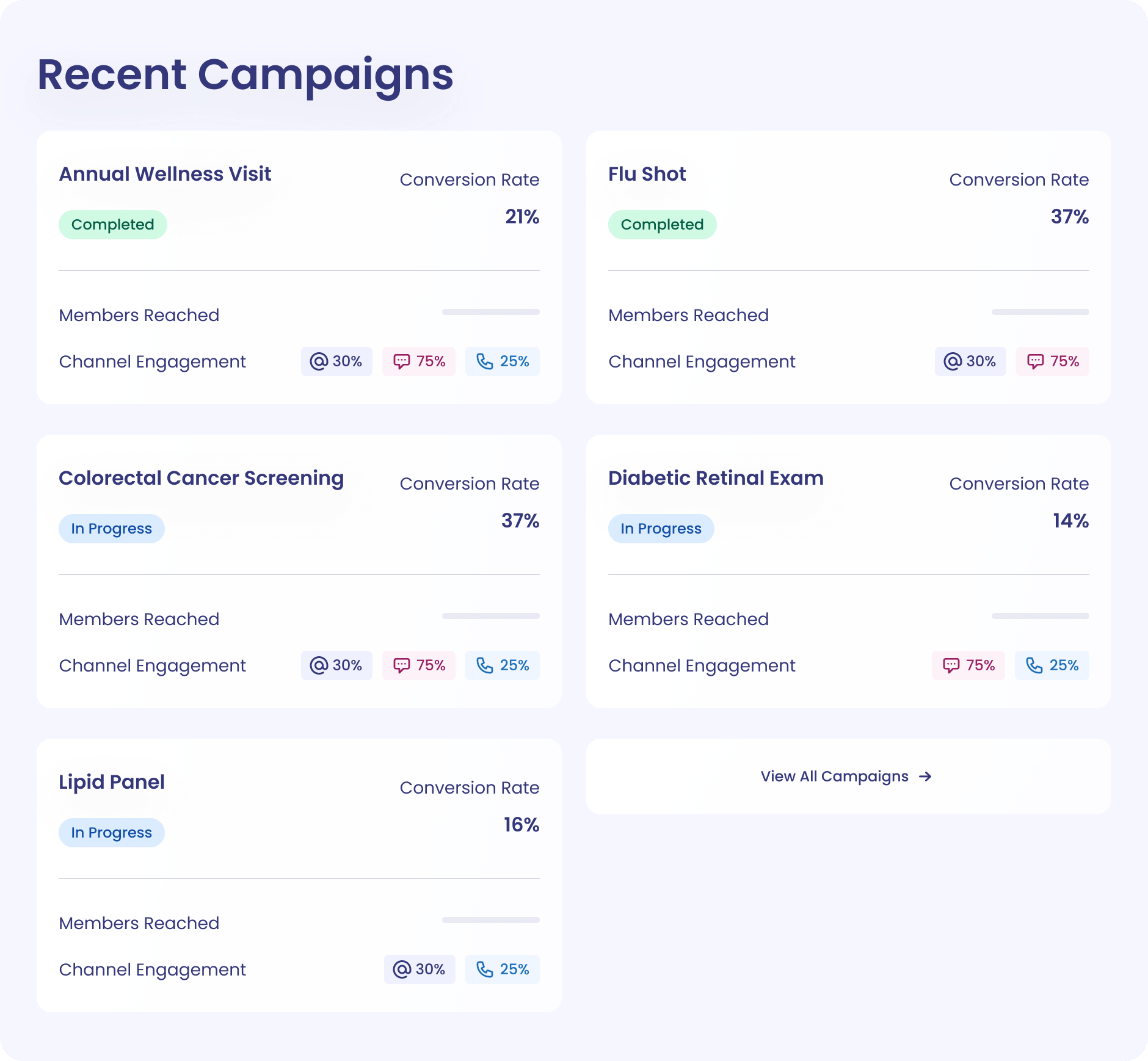
Data that drives action
Access member data, including demographics, care gaps and social risk factors, all in one place. We get the full picture of each member to create an experience tailored to each member’s needs and barriers.

Coordinated connection
Eliminate patient abrasion and confusion by centralizing member outreach in one platform. By creating a simplified communication strategy that meets the goals of different departments, we help you encourage members to take action, helping to close care gaps and improve health outcomes.
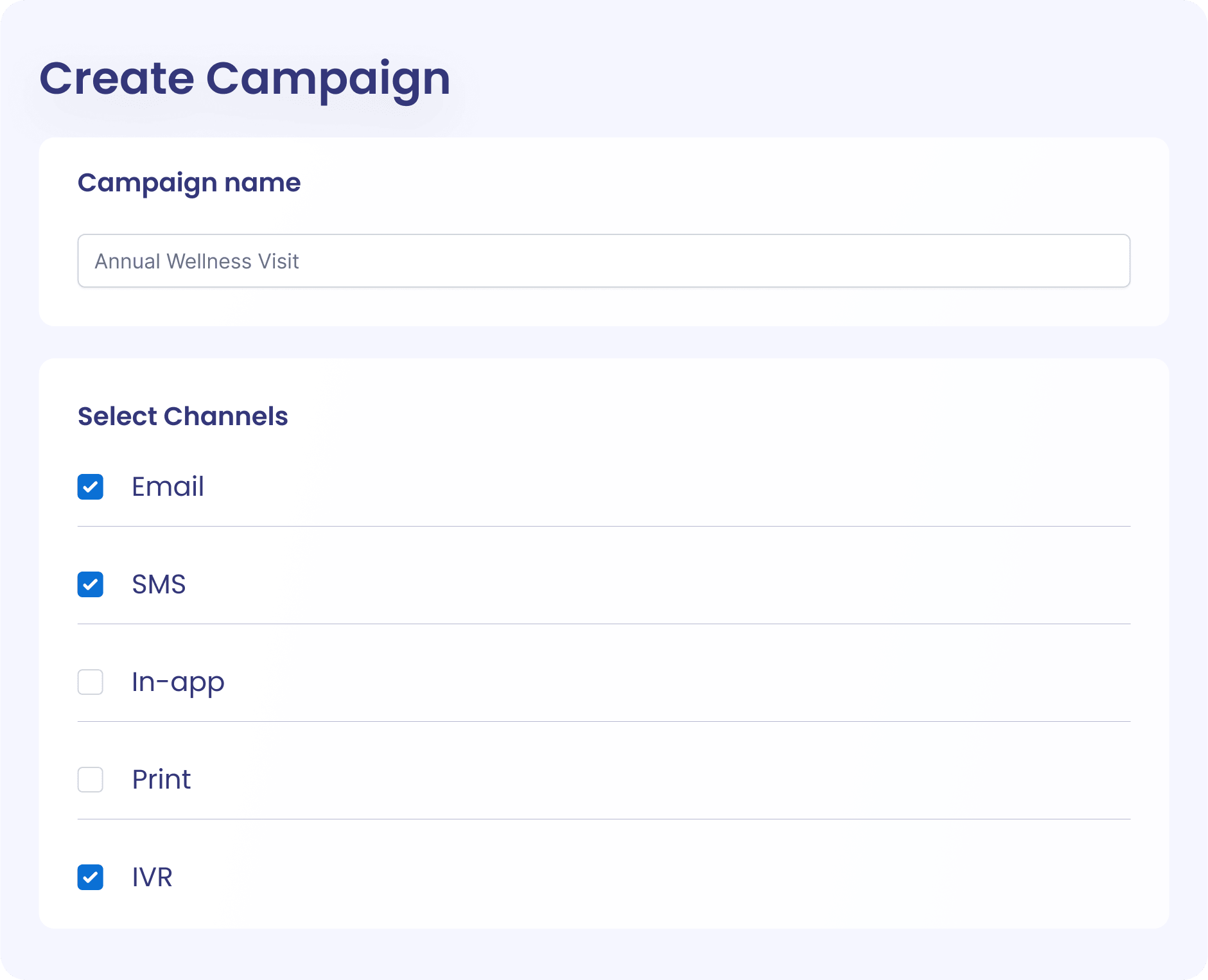
Personalization at scale
Whether you’re targeting 5 or 5000 members, you’re able to tailor experiences to each member’s health condition and risk factors so they feel seen and heard by their plan, building trust and increasing member satisfaction over time.

Simplified workflow
Streamline your team’s workflow through automation and integrated communication. We provide relief to health plan teams by taking care of the details so your team can focus on the big picture of each member’s personalized experience.
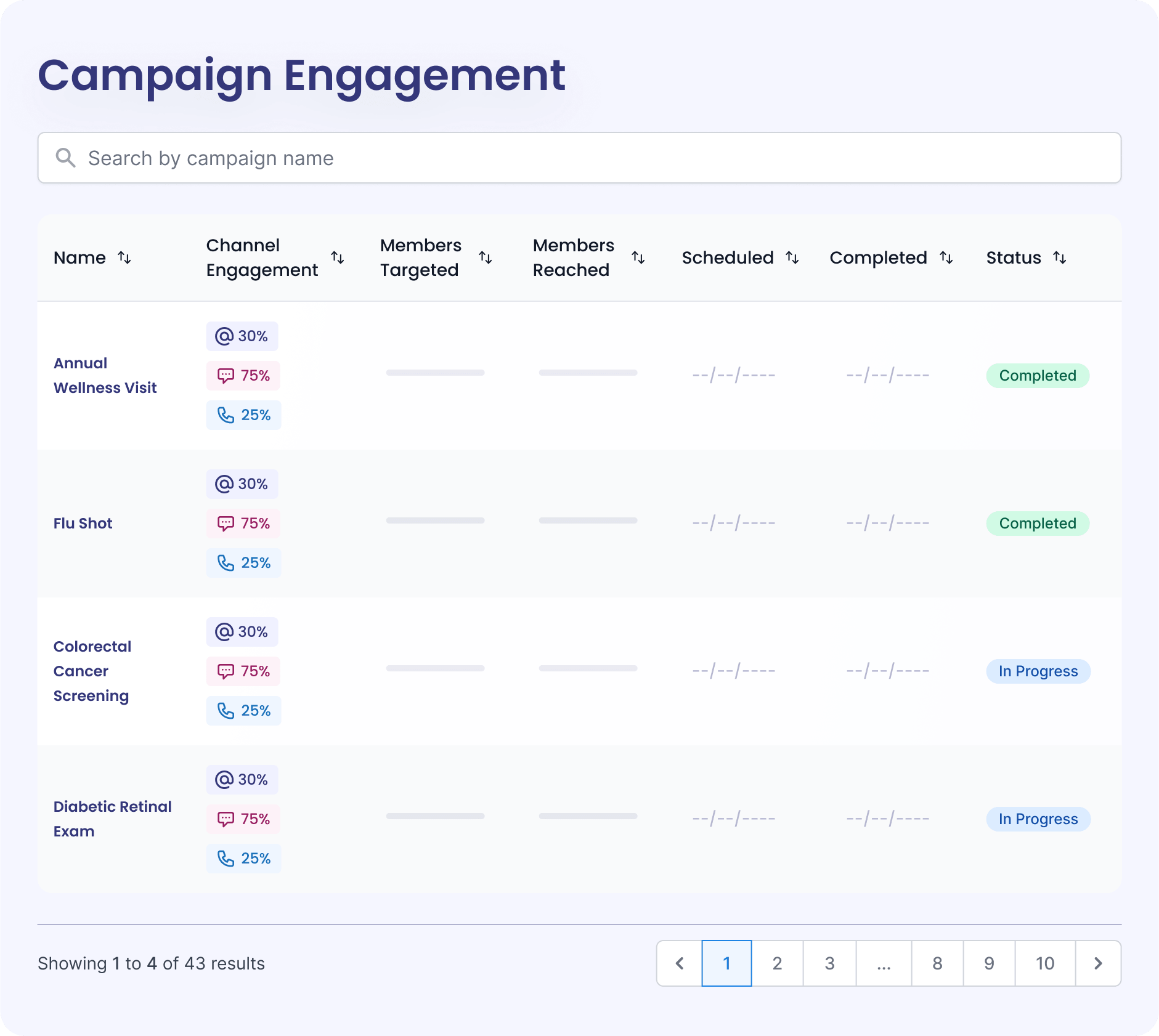
Compliance made easier
We help you keep up with ever-changing regulations and maintain CMS-compliant member outreach. Our advanced data tools allow you to track member outreach so you can ensure you’re doing your due diligence to get members to the right type of care.
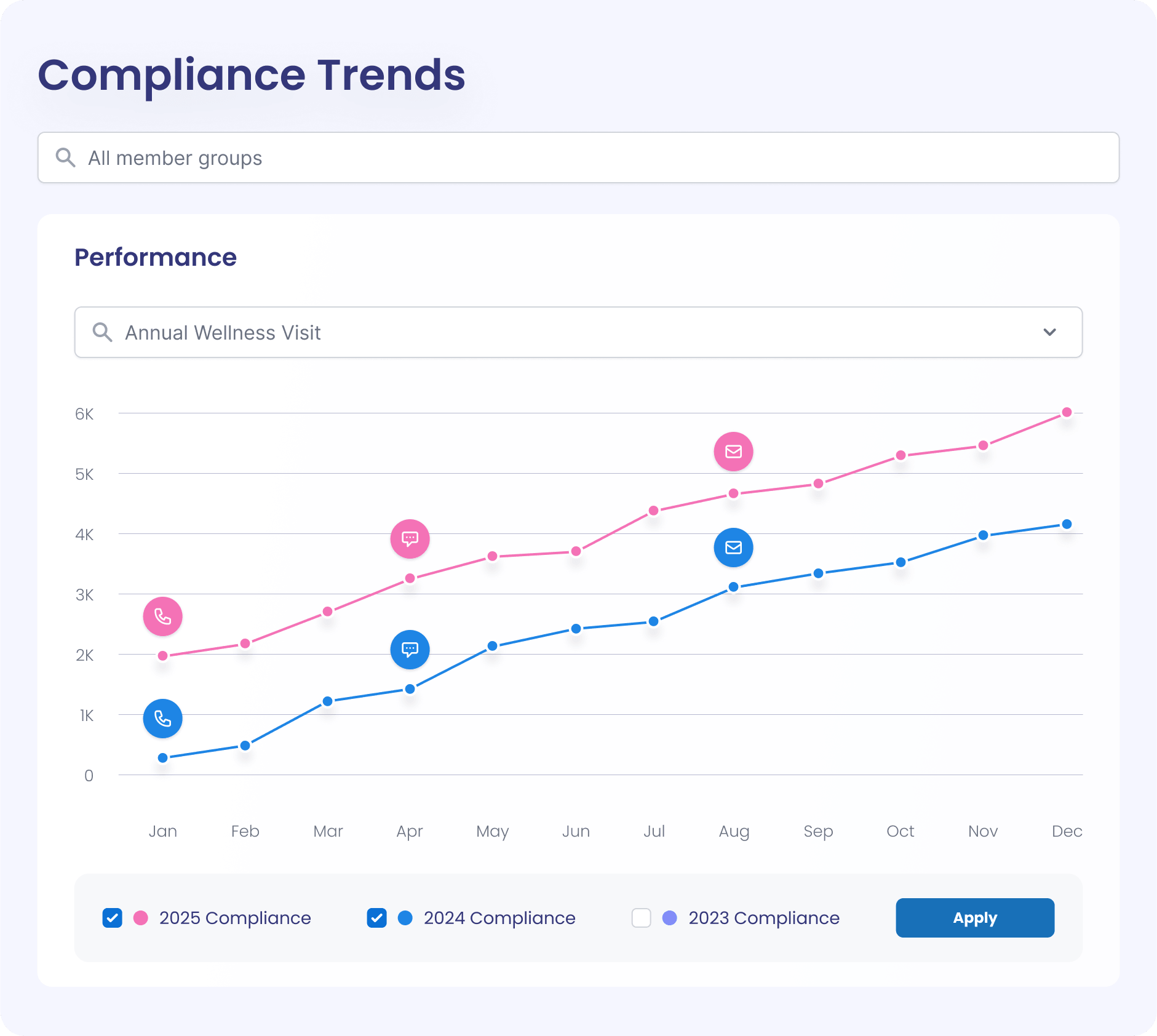






by the numbers
Results that matter
QRM gives plans a clear path towards performance improvement, without increasing costs.
Engagement that matters
A platform designed just for health plans
Simplify engagement at every step in your members' care journeys.








Meaningful Automation
Technology that works together
Our platform empowers health plans to create tailored member experiences to engage, manage, optimize – and repeat. Better member experiences result in better data for your team, creating a dynamic cycle that benefits members and health plan teams.


.webp)

